1.) What is gout?
Gout is a form of inflammatory arthritis classified as a crystal-induced arthropathy. It is caused by the deposition of monosodium urate (MSU) crystals in joints, soft tissues, and sometimes other sites, resulting from chronic hyperuricemia (elevated serum urate levels >6.8 mg/dL). Excess urate (from overproduction or underexcretion of purine metabolism end-products) leads to MSU crystal formation causing acute flares. Key impacts include recurrent painful attacks, potential progression to chronic tophaceous gout with joint damage, deformity, and disability, plus associations with comorbidities like cardiovascular disease, kidney stones, and chronic kidney disease.
2.) Key Signs and Symptoms
- Hallmark symptoms:
- Sudden, severe pain (often described as excruciating)
- Swelling, erythema (redness), warmth, and tenderness in the affected joint
- Peak intensity within 24 hours; commonly monoarticular
- Systemic manifestations: Fever (especially in polyarticular flares), malaise, chills
- Extra-articular involvement: Tophi (subcutaneous urate deposits, e.g., ears, olecranon, fingers), kidney stones (uric acid nephrolithiasis), chronic arthropathy with joint destruction
3.) Risk Factors:
- Genetic
- Family history, genetic variants affecting urate transport and renal excretion
- Environmental:
- Medications (diuretics like thiazides/furosemide, low-dose aspirin)
- Dehydration, lead exposure
- Demographic:
- Male sex
- Older age
- Postmenopausal women
- Lifestyle:
- Diet high in purines (red meat, organ meats, shellfish, fructose-rich drinks)
- Alcohol (especially beer)
- Obesity
- Sedentary lifestyle
- Medical Conditions
- Untreated high blood pressure
- Diabetes
- Obesity
- Metabolic syndrome
- Heart disease
- Kidney disease
4.) Diagnosis
- History and Physical
- History of joint pain, swelling, redness-frequency, severity, number of involved joints, what has worked
- Joint exam
- Labs:
- Serum urate >6.8 mg/dL. However, may be normal during acute flare
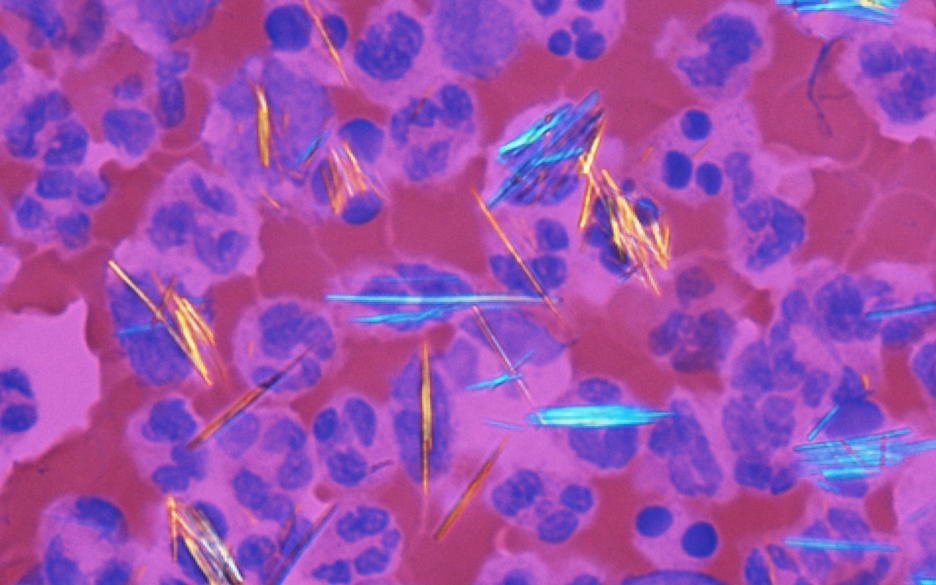
- Synovial fluid analysis using polarized light microscopy (gold standard: needle-shaped, negatively birefringent MSU crystals)
- Inflammatory markers (elevated WBC, ESR, CRP during flare)
- Imaging:
- Ultrasound (double contour sign on cartilage, tophi, effusions)
- Dual-energy CT (DECT)
- Plain X-rays (late: punched-out erosions with overhanging edges, tophi)
- Clinical criteria:
- ACR/EULAR classification criteria (score-based: entry criterion of ≥1 episode of swelling/pain/tenderness in peripheral joint/bursa; points for MSU crystals, tophi, typical podagra, rapid onset, etc.; ≥8 points classifies as gout)
5.) Treatment Goals
- Rapidly resolve acute flares and control pain/inflammation
- Prevent recurrent flares
- Achieve and maintain serum urate <6 mg/dL (treat-to-target strategy)
- Dissolve tophi and prevent joint damage/deformity
- Minimize comorbidities and improve quality of life
6.) Medications
- Symptom Relief (for acute flares):
- NSAIDs
- Colchicine
- Corticosteroids (oral, intra-articular, or systemic)
- Purified corticotrophin injections
- IL-1 inhibitors (e.g., anakinra) for refractory cases
- Conventional / Foundational:
- Xanthine oxidase inhibitors (block body’s production of uric acid): Allopurinol (first-line, start low dose especially in CKD) or febuxostat.
- Uricosurics(increase renal excretion of urate): Probenecid (only if normal renal function)
- Biologic Therapies:
- Pegloticase (IV uricase enzyme) for refractory/uncontrolled gout with persistent high urate, frequent flares, or tophi
- Flare prophylaxis (low-dose colchicine or NSAID) when starting ULT
7.) Management & Nursing Considerations
- Physical Activity & Lifestyle:
- Encourage weight loss if obese, regular low-impact exercise (once flare resolves), hydration (2-3 L/day)
- Low-purine diet: limit red meat, shellfish, alcohol (especially beer), sugary drinks; emphasize vegetables, low-fat dairy, cherries/vitamin C
- Patient Education:
- Explain disease as treatable chronic condition; stress adherence to ULT to prevent flares/damage
- Recognize flare triggers (diet, dehydration, injury) and early signs
- Teach medication adherence, including prophylaxis to avoid mobilization flares and continuing urate lowering therapy during flares.
- Monitoring:
- Serial serum urate (target <6 mg/dL)
- Renal function, CBC, liver tests (for ULT side effects)
- Joint assessment for tophi, deformity; monitor for infection in flares
- Emotional Support:
- Acknowledge severe pain impact on mobility/mood; provide empathy, refer to support groups if needed
8.) Definitions & Key Terms
- Hyperuricemia — Elevated serum urate (>6.8 mg/dL), precursor to gout but not always symptomatic
- Monosodium urate (MSU) crystals — Needle-shaped crystals from urate deposition that trigger inflammation
- Podagra — Classic acute gout attack in the first metatarsophalangeal joint (big toe)
- Tophus/tophi — Subcutaneous or intra-articular deposits of aggregated MSU crystals
- Treat-to-target — Strategy of titrating ULT to achieve/maintain serum urate <6 mg/dL
- Flare — Acute inflammatory episode due to crystal shedding/immune response
- Urate-lowering therapy (ULT) — Medications to reduce serum urate
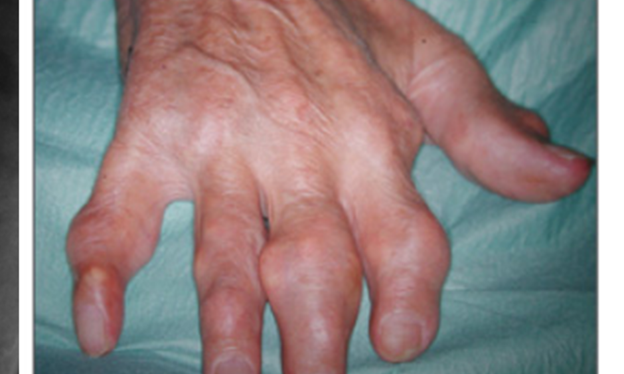
https://www.emjreviews.com/wp-content/uploads/2017/11/Figure-2-Tophaceous-gout-of-the-hand.png
Monosodium Urate Crystals
References
- Mayo Clinic. (2022, November 16). Gout – Diagnosis and treatment. https://www.mayoclinic.org/diseases-conditions/gout/diagnosis-treatment/drc-20372903
- Arthritis Care & Research Vol. 72, No. 6, June 2020, pp 744–760 DOI 10.1002/acr.24180 © 2020, American College of Rheumatology

